From Setup to Sleeping Comfortably — A Simple Step‑by‑Step Guide from A Real CPAP User
Introduction
I’m Really Glad You Found This
If you’re reading this, there’s a very good chance you’re overwhelmed.
I know I certainly was!
Maybe you’ve just been diagnosed with sleep apnea and you’re still trying to process what that even means. Maybe you recently brought a CPAP machine home and it’s sitting on your bedside table right now, quietly waiting for tonight. Maybe you tried it once and already feel discouraged.
You might be thinking:
“I can’t breathe in this thing.”
“This feels unnatural.”
“What if I never get used to it?”
“What if I fail at this?”
Before we go any further, pause.
Take one slow breath in.
And let it out slowly.
Nothing about how you’re feeling right now is unusual.
You are not weak for feeling anxious.
You are not dramatic for feeling unsettled.
You are not failing because it feels hard.
You are human.
I know this because I was exactly where you are.
When I was diagnosed, I felt two things at the same time: relief and fear.
Relief — because there was finally an explanation for the constant exhaustion, the brain fog, the morning headaches, the feeling of never truly feeling rested.
Fear — because I was told I would need a machine to breathe at night.
A machine!
The pickup appointment was efficient. The technician explained the buttons, fitted the mask, adjusted straps, and showed me how to fill the humidifier (which was not included). I nodded along, trying to absorb everything.
Then I went home.
And that night, sitting on the edge of my bed holding the mask in my hands, it all hit me.
This wasn’t theoretical anymore.
This was real.
Honestly it was overwhelming.
The first time I turned the machine on and put the mask to my face, my body reacted instantly. My breathing felt mechanical. The air pressure felt strange. I became hyper‑aware of every inhale and exhale.
Within seconds my thoughts spiralled:
“This isn’t normal.”
“I can’t relax like this.”
“There’s no way I can sleep like this.”
I pulled the mask off.
No one had warned me about that part.
No one had prepared me for the emotional side of starting CPAP — the vulnerability of sleeping with equipment, the anxiety of forced airflow, the strange psychological adjustment of relying on a device to breathe well.
What I eventually learned — slowly, imperfectly — was this:
What I was feeling was completely normal.
The panic was not proof I couldn’t adapt.
The discomfort was not permanent.
The fear was part of the adjustment process.
Gradually, the sharp edges softened.
What felt alarming became tolerable.
What felt tolerable became familiar.
What felt familiar eventually became routine.
This guide is what I wish someone had calmly explained to me during that first week.
No overwhelming medical jargon.
No unrealistic promises.
No pressure to “just get used to it.”
Just steady reassurance and practical steps that move you from fear to confidence — at a human pace.
You don’t have to master this tonight.
You only have to take the next small step.
And then another tomorrow.
Medical Disclaimer
This guide is for informational and educational purposes only.
I am not a physician, sleep specialist, respiratory therapist, or licensed medical professional. The content in this guide is based on personal experience combined with widely available general information about CPAP therapy.
It is not intended to diagnose, treat, cure, or prevent any medical condition.
Always follow the guidance of your healthcare provider regarding pressure settings, equipment adjustments, and treatment decisions. Never change prescribed pressure settings or discontinue therapy without consulting your provider.
If you experience chest pain, severe breathing difficulty, persistent discomfort, or any concerning symptoms, seek medical advice from a qualified healthcare professional.
You are responsible for your own health decisions, and this guide does not replace professional medical care.
PHASE 1 – CALMING THE PANIC
When Everything Feels Overwhelming
The beginning is often the hardest part — not because CPAP is impossible, but because it disrupts something deeply personal: sleep.
Sleep is when we are most vulnerable.
And now you’re being asked to trust a machine during that vulnerable state.
Of course, your nervous system reacts.
Step 1 – You’re Not Weak for Feeling This Way
Let’s say this clearly:
You’ve been told you stop breathing at night.
You’ve been handed medical equipment.
You’ve been expected to adapt quickly.
That is a lot for anyone.
Your brain’s primary job is to keep you safe. When something unfamiliar covers your face and pushes air into your airway, your nervous system evaluates it as a potential threat.
That reaction can look like:
“I can’t relax.”
“This feels wrong.”
“I need to take this off right now.”
That is not failure.
That is your nervous system doing its job.
Your brain is not rejecting CPAP.
It is trying to understand it.
Learning requires repetition.
Right now, your only job is exposure — not perfection.
If you wear it for ten minutes, that is exposure.
If you turn it on and sit upright reading, that is exposure.
If you fall asleep with it for an hour, that is exposure.
I honestly could not put the mask over my face at all so if that’s you then don’t panic.
Each exposure teaches your brain:
“This is safe.”
And safety reduces panic.
Step 2 – Understanding Your Diagnosis Without Spiralling
The language around sleep apnea can sound frightening.
“Moderate.”
“Severe.”
“High AHI.”
“Oxygen desaturation.”
It’s easy for your mind to jump from those words to catastrophic conclusions.
But here’s what those classifications actually mean:
They describe frequency — not doom.
They measure how often breathing is interrupted during sleep.
They do not predict your future.
They do not mean your body is irreparably damaged. They do not mean something terrible is about to happen.
Sleep apnea is common.
Millions of people have it.
It is highly treatable.
CPAP therapy is one of the most researched and effective treatments in sleep medicine.
You were not diagnosed because something is hopeless.
You were diagnosed because something is manageable — and now it’s being managed.
Instead of thinking:
“This is severe. This is terrible.”
Try shifting to:
“This is treatable. And I am treating it.”
That shift alone lowers anxiety.
You are not ignoring the problem.
You are addressing it.
That matters.
It might not feel like it just now, but I promise you that you are now in a much better position.
Step 3 – Why the Pickup Appointment Feels So Fast
Almost everyone has the same experience.
You go to collect your CPAP machine. The technician explains the buttons, shows you how to assemble the mask, talks about humidity settings, maybe mentions compliance requirements — and then it’s over.
You walk out with a machine in a bag.
Later that evening, you realise something uncomfortable:
You don’t remember half of what was said.
This is incredibly common. My experience was, where do these straps go? How do I get the mask on, where does this tube attach. It felt desperately hopeless.
When we’re stressed, our brains prioritise emotional processing over memory storage. Being told you stop breathing at night — even calmly — activates stress. Stress reduces information retention.
It doesn’t mean you weren’t paying attention.
It doesn’t mean you’re bad with instructions.
It means you were processing something significant.
You are not behind.
You are learning something new, and learning happens through repetition — not one appointment.
If you need to watch tutorials, reread instructions, or ask questions later, that’s not incompetence. That’s reinforcement. That’s normal.
Step 4 – Lowering the Bar for Success
Many new CPAP users silently create an impossible rule:
“If I can’t wear it all night immediately, I’m failing.”
Beware of this and take a moment to address this, this is super important and completely not true.
That belief creates pressure.
Pressure creates anxiety.
Anxiety makes sleep harder.
So let’s remove that rule entirely.
Tonight, success might be:
20 minutes.
45 minutes.
One sleep cycle.
Putting it back on after waking up.
For me it was simply putting the mask on my face for a few seconds.
All of that counts.
Adaptation is not about intensity. It’s about consistency.
Wearing it for a short period every night teaches your nervous system that the mask is not a threat. Forcing eight straight hours on night one often backfires.
Small, repeatable wins build long‑term success.
Lowering the bar doesn’t lower your standards.
It builds resilience.
But this is where I can really help.
What I did for a few days was just attempt to wear the mask for 30 seconds at a time while sitting up in any other room than your bedroom and watching TV as a distraction.
This alone massively took the pressure off me mentally and actually wearing it just for a few minutes sat up during the day was the key to everything.
Step 5 – Managing Claustrophobia Gently
Claustrophobia is one of the most common early reactions to CPAP.
It is not weakness.
It is not immaturity.
It is your brain reacting to perceived loss of control.
When something covers your nose or face and alters airflow, your nervous system can interpret it as confinement.
The solution is gradual exposure — not force.
Once you have grown comfortable with wearing during the day,
Instead of trying to fall asleep immediately:
Sit upright.
Keep the lights on.
Put the mask on for one minute.
Breathe slowly and deliberately.
Then take it off.
Do this daily.
Then extend it to two minutes.
Then five.
You are not trying to prove anything. You are retraining your nervous system.
Each calm repetition sends a signal:
“This is safe. I can remove it anytime.”
Control reduces panic.
And repetition builds calm.
If I could only give one piece of advice, then this would be it.
PHASE 2 – MAKING IT MORE COMFORTABLE
Reducing the Friction
If you’re reading this section, it means you didn’t quit.
That matters. Even if you still feel like you are failing, you simply are not,
Most successful long‑term CPAP users did not succeed immediately. They struggled. They adjusted. They experimented. They learned.
They stayed.
This phase is about reducing the small annoyances that create resistance.
Step 6 – Taking the Mask Off in Your Sleep
You may wake up in the middle of the night and realise your mask is on the pillow beside you.
Your first thought might be:
“I failed.”
You didn’t.
Your unconscious brain removes unfamiliar objects during sleep. Especially in the early weeks.
Think of it this way:
Your waking brain agreed to wear the mask.
Your sleeping brain hasn’t fully caught up yet.
Each night you wear it — even partially — your brain gathers evidence:
“That was safe.”
“I could breathe.”
“Nothing bad happened.”
Over time, familiarity reduces removal.
If you wake up and it’s off, calmly put it back on if you can.
No frustration.
No self‑criticism.
Just repetition.
It’s no big deal, eventually one morning you will wake up with the mask on. Reward yourself on that day!
Step 7 – Stop Overtightening the Mask
When you feel or hear a leak, your instinct may be to tighten the straps.
Tighter feels more secure.
But tighter is not always better.
Most CPAP masks are designed to inflate slightly with air pressure. That inflation helps create the seal. If you overtighten, you can actually distort the cushion and increase leaks.
Overtightening also creates:
Pressure marks
Facial soreness
Headaches
More resistance to wearing it
Instead of pulling straps tighter, try:
Reseating the mask gently
Adjusting while lying down
Allowing the cushion to inflate naturally
Comfort improves compliance.
Force increases frustration.
What I do is put the mask in position on my face and then turn on the air, I feel this gives me a better seal.
Step 8 – Mask Leaks Are Mechanical, Not Personal
Leaks are one of the most common frustrations.
They can sound loud.
They can blow air into your eyes.
They can wake your partner.
It’s easy to interpret leaks emotionally:
“I can’t even wear this properly.”
But leaks are mechanical problems.
And mechanical problems have mechanical solutions.
It may mean:
The mask size isn’t ideal.
The cushion needs replacing.
The straps need minor adjustment.
Your sleeping position shifted.
None of those mean you’re incapable.
You’re learning equipment.
Learning always involves adjustment.
I currently use a ResMed F20 as its super simple.
This is purely personal preference but don’t put up with leaks.
There are tons of options to try. I just want something that covers my nose and mouth with a good seal.
Check out the ResMed F20 mask here on Amazon
(Click the blue links and it takes you to Amazon)
https://geni.us/4MGFu6s (Amazon)
(As an Amazon associate, I earn from qualifying purchases)
And if strap marks are a problem check out this solution,
Pad A Cheek
https://www.padacheek.com
Step 9 – Dry Mouth and Humidity Issues
Waking up with a dry mouth can feel discouraging.
Common causes include:
Mouth breathing
Low humidity settings
Dry bedroom air
Instead of changing everything at once, adjust one variable at a time.
Increase humidity slightly.
Observe for a few nights.
Then reassess.
Systematic adjustment builds confidence.
You move from feeling helpless to feeling capable.
And that psychological shift is powerful.
This hurdle takes consistency to overcome.
When I receive my CPAP machine (Resmed Airsense 10) It did not include the humidifier chamber, once I added this it greatly reduced dryness by adding a small amount of humidity to the air,
Check out the ResMed AirSense 10 and 11 Humidifiers below.
https://geni.us/Z03Qa (Amazon) AirSense10
https://geni.us/l7L2aHe (Amazon) AirSense 11
As an Amazon Associate, I earn from qualifying purchases)
The final piece of the puzzle for me though was purchasing a heated tube.
A heated CPAP tube helps prevent condensation (“rainout”) in the hose while maintaining consistent warm airflow, which reduces dryness, nasal irritation, and sudden bursts of water in the mask for a more comfortable night’s sleep.
You can control the air temperature, and this really helps with comfort.
Check out the heated tube below
https://geni.us/pwVwsB (Amazon) ResMed AirSense 10
https://geni.us/AEE42 (Amazon) ResMed AirSense 11
(As an Amazon Associate, I earn from qualifying purchases)
Step 10 – Air in the Stomach (Aerophagia)
Some people experience bloating or mild stomach discomfort in the early weeks.
This can happen when air is swallowed during adaptation.
It often improves as:
Your body adjusts to pressure
Your breathing becomes more relaxed
Your anxiety decreases
Mild early discomfort does not mean damage.
It usually means adaptation.
If it persists or is severe, consult your provider — but early temporary bloating is common and often resolves naturally.
Let’s just say a little extra gas is inevitable!
Step 11 – Hose Management Matters More Than You Think
The hose can feel surprisingly intrusive.
Dragging across the bed.
Pulling when you turn.
Getting tangled.
Small setup changes can make a big difference.
You Could Try:
Routing the hose above your head
Using a hose holder
Clipping it to the headboard
Positioning it so it moves freely
When physical resistance decreases, emotional resistance often decreases too.
Comfort is cumulative.
What I do to avoid “Rainout” is put the machine near the floor lower than my sleeping position, along with a heated tube this helps with “Rainout”
Rainout is when warm, humidified air from your CPAP cools inside the hose and turns back into water droplets, causing moisture to collect in the tubing or mask. You don’t want rainout because it can lead to gurgling noises, water splashing into your mask, disrupted sleep, and reduced comfort throughout the night.
If you don’t have a heated tube a cheaper option is a hose cover to keep the tube a little warmer. This may be enough depending on your settings and set up to avoid rainout,
Check out the cover I use below
https://geni.us/wYlcD (Amazon)
(As an Amazon associate, I earn from qualifying purchases)
PHASE 3 – BUILDING CONFIDENCE
When It Starts Feeling Manageable
At some point — often quietly — something begins to shift.
The panic isn’t as sharp.
The mask doesn’t feel quite as foreign.
You stop bracing yourself every time you turn the machine on.
This phase is subtle but important.
You move from reacting…
to participating.
Instead of thinking, “I hope I survive this night,”
you begin thinking, “How can I make this work better?”
That shift is confidence forming.
Step 12 – Create a Simple Night Routine
Predictability calms the nervous system.
When your brain knows what comes next, it relaxes more easily.
Instead of treating CPAP as an interruption, integrate it into a consistent pre‑sleep sequence.
For example:
- Wash your face
- Fill the humidifier
- Check the mask cushion
- Put the mask on
- Turn the machine on
- Take one slow breath in, one slow breath out
Follow the same order each night.
Over time, the routine itself becomes a cue for sleep.
The mask stops feeling like a disruption.
It becomes part of the ritual.
And rituals are calming.
Step 13 – Keep Cleaning Simple and Sustainable
In the beginning, it’s easy to become overly strict.
You might feel like you need to deep clean everything constantly or you’re “doing it wrong.”
Perfection is not required.
Sustainability is.
A simple approach works well:
• Quick wipe of the mask cushion daily
• Regular wash of mask and tubing
• Replace worn cushions and filters as needed
You don’t need elaborate systems.
You need repeatable systems.
When maintenance feels manageable, resistance decreases.
Here’s what I do.
I clean the hose every 3 days, run some dish soap and water through and a cpap cleaning hose brush.
For the humidity chamber I do this daily. I clean with water and dish soap and use a toothbrush to clean the inner.
For the mask cushion I use a bar of soap (Imperial leather brand)
What I found at first is that if I used a CPAP wipe or forgot to clean the mask all together it led to more leaks. This is due to the mask sliding.
Washing with a bar of soap (daily) gives the cushion surface the correct grip again)
Step 14 – Understand Just Enough
You don’t need to become a sleep technician.
But understanding a few key concepts reduces helplessness.
For example:
AHI – how many breathing interruptions occur per hour
Leak rate – whether your mask is sealing effectively
Humidity – how moisture affects comfort
When you understand what these mean, you stop guessing.
You start interpreting.
You move from:
“Something feels wrong.”
To:
“I know what this number means.”
Knowledge replaces uncertainty.
And uncertainty is what fuels anxiety.
Step 15 – Tracking Progress Without Obsessing
Most CPAP machines track basic data:
• AHI
• Leak rate
• Usage hours
You may view this on the machine itself or through software platforms like SleepHQ or OSCAR.
Seeing improvement can be incredibly encouraging.
Lower AHI numbers.
Longer usage hours.
Fewer leaks.
Data becomes reassurance.
But here’s the balance:
Look at trends — not single nights.
Sleep varies.
Stress affects results.
Illness affects results.
Travel affects results.
One imperfect night does not erase progress.
Consistency over weeks matters more than perfection over one evening.
Sleep HQ has a user-friendly dashboard that shows your daily information and trend data over time.
There is a free trial, and the community is incredibly helpful.
You can visit SleepHQ here, https://www.sleephq.com/
Daily Dashboard (My data)
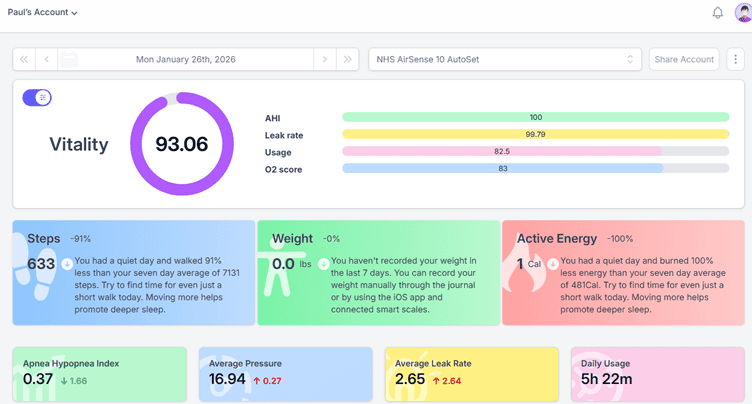
Trend data.
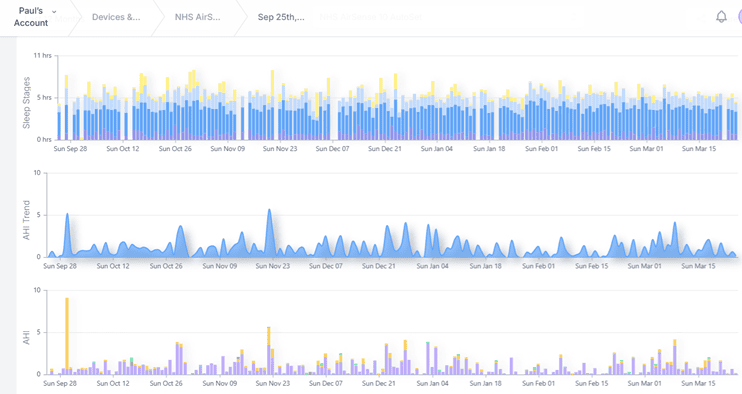
Step 16 – Notice Subtle Improvements
Improvements are sometimes quiet.
You may not wake up feeling dramatically different.
Instead, you might notice:
You’re thinking more clearly mid‑morning.
You’re not reaching for caffeine as desperately.
Your mood feels steadier.
You’re not crashing in the afternoon.
These changes can be gradual.
Pause when you notice them.
Your brain needs to register success.
When you consciously acknowledge improvement, motivation strengthens.
Step 17 – Let Yourself Feel Hopeful
There may come a morning — unexpectedly — when you wake up and think:
“I actually feel… okay.”
Not euphoric.
Not transformed.
Just… okay.
Rested enough. Clear enough.
That moment is powerful.
Because it proves something:
This is working.
CPAP shifts from being a burden you tolerate…
to support your value.
And that psychological transition changes everything.
PHASE 4 – LONG‑TERM CONFIDENCE
When It Becomes Normal
There will be a night when you put the mask on without debating it.
No internal argument.
No tension in your shoulders.
No countdown in your head.
You just put it on.
Like brushing your teeth.
That’s not surrender.
That’s adaptation.
Step 18 – From Patient to Capable
At this stage, something subtle changes in identity.
You no longer feel like someone “dealing with a condition.”
You feel like someone managing their health.
You understand your machine.
You know how to adjust comfort settings.
You recognise normal variations.
You feel capable.
Capability replaces fear.
Step 19 – Bad Nights Still Happen
Even experienced users have rough nights.
Stress.
Illness.
Congestion.
Travel.
Life.
A single bad night does not undo months of consistency.
Progress is not erased by imperfection.
Stay steady.
Consistency over time is what matters. Don’t blame CPAP for every future symptom you get. They might have happened anyway,
Step 20 – Travel With Confidence
The first time you travel with your CPAP, it may feel awkward.
You may feel self‑conscious carrying it.
But something interesting happens over time:
You realise how much better you sleep with it.
You start packing it automatically.
You prioritise your rest.
That’s growth.
You move from embarrassment to ownership.
Also, I will add that CPAP machines do not count as carry on luggage, so take onboard with you alongside your carry on luggage,
Step 21 – Letting Go of Shame
There is nothing shameful about treating a medical condition.
Millions of people use CPAP.
Athletes. Professionals. Parents. Partners.
Health maintenance is not weakness.
It is responsibility.
Confidence replaces self‑consciousness when you remember:
You are taking care of yourself.
Step 22 – Look How Far You’ve Come
Think back to the first night.
The uncertainty.
The panic.
The doubt.
Now look at where you are.
You stayed.
You adjusted.
You learned.
That is resilience.
Not dramatic resilience.
Quiet resilience.
And quiet resilience is powerful.
Step 23 – Energy Returning
As breathing stabilises during sleep:
Oxygen levels stabilise.
Micro‑awakenings decrease.
Deep sleep becomes more consistent.
The benefits compound gradually.
You may feel:
Clearer thinking
More stable mood
Improved concentration
Greater patience
Energy doesn’t always return in a dramatic rush.
Sometimes it builds quietly.
But it builds.
Step 24 – When You Know It’s Working
There is often a simple moment.
A quiet morning.
You wake up and think:
“I’m glad I stuck with this.”
That thought signals a turning point.
The machine is no longer the enemy.
It is support.
Step 25 – This Is Sustainable
CPAP is not a temporary test of endurance.
It becomes routine.
Normal.
Integrated.
Like wearing glasses.
Like using a seatbelt.
Like brushing your teeth.
At first it feels intrusive.
Eventually, it just feels sensible.
And normal is powerful.
Step 26 – You’re Stronger Than You Thought
You faced something that scared you.
You adapted to something uncomfortable.
You didn’t quit on the hard nights.
That’s strength.
Not loud strength.
Steady strength.
And steady strength lasts.
Step 27 – Hope Moving Forward
The intensity of the beginning does not last forever.
Panic softens.
Equipment becomes familiar.
Resistance fades.
Confidence replaces doubt.
Adaptation is one of the most reliable traits of the human nervous system.
Given repetition and safety, it adjusts.
You are adjusting.
Even when it feels slow.
Even when it feels imperfect.
Adaptation works.
Step 28
What If CPAP Isn’t Working and I Still Feel Tired?
If you’re using your CPAP consistently but still waking up tired, foggy, or discouraged, there is one simple step that can give you real clarity:
Start tracking your overnight oxygen levels.
The entire purpose of CPAP therapy is to keep your airway open so your oxygen stays stable throughout the night. When oxygen repeatedly drops — even briefly — your body goes into stress mode. Your heart rate increases. Your brain partially wakes. Deep sleep gets disrupted. And the result is simple: you still feel exhausted.
You cannot feel oxygen levels.
You cannot guess oxygen stability.
You have to measure it.
That’s where an O₂ ring becomes incredibly valuable.
Unlike most smartwatches, which measure oxygen only periodically, a dedicated O₂ ring tracks your oxygen continuously throughout the entire night. It stays securely on your finger and records detailed trends, including short desaturations that can easily be missed otherwise.
Instead of lying in bed wondering:
“Is this working?”
“Why am I still tired?”
“Is something wrong?”
You wake up with answers.
You can see:
- Whether your oxygen stayed stable
- Whether drops are still happening
- Whether things are improving over time
That clarity alone reduces anxiety.
For me personally, this was the turning point. I stopped guessing and started measuring. When I began monitoring my oxygen nightly, I could actually see progress. As my oxygen levels became more stable, I started feeling clearer and more consistent during the day.
It wasn’t dramatic.
It wasn’t instant.
But it was measurable.
And measurable progress builds confidence.
If you are serious about understanding whether your CPAP therapy is truly working, an O₂ ring is one of the most empowering tools you can add. It turns uncertainty into data. It turns doubt into direction.
This vibrates if your blood oxygen drops below a certain level, You can turn this off as well though.
What I did at the beginning of my CPAP journey is I wore the 02 Sensor overnight with out cpap.
Here is the result (First Night No CPAP)
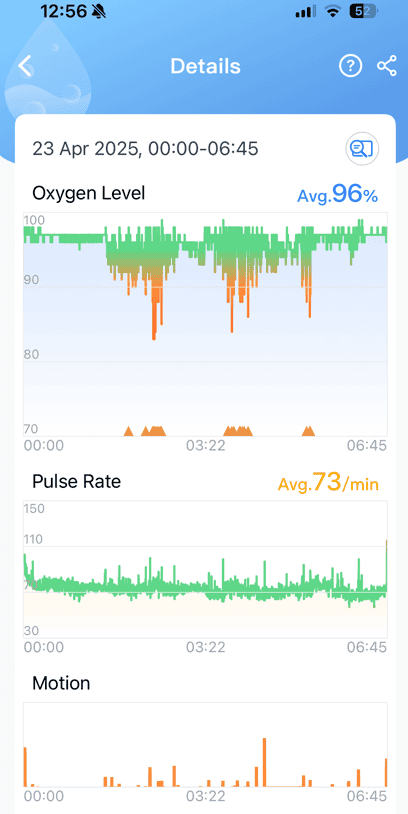
And here is my result today, (11 months apart)

Check out the O2 ring here https://geni.us/WHNVxu (Amazon)
Sometimes the difference between “CPAP isn’t working” and “CPAP is helping” is simply having the right information in front of you.
An O₂ ring gives you that information.
The combination of this and the helpful forum on SLEEPHQ and all the data got me to this point.
Helpful Resources
SleepHQ
https://sleephq.com
OSCAR (Free CPAP Data Software)
https://www.sleepfiles.com/OSCAR/
Pad A Cheek
https://www.padacheek.com
CPAP Reviews (Nick)
https://www.youtube.com/@CPAPReviews
TheLankyLefty27
https://www.youtube.com/@TheLankyLefty27
FreeCPAPAdvice
https://www.youtube.com/@FreeCPAPAdvice
Final Words
If you take nothing else from this guide, take this:
The discomfort of the beginning is not a prediction of the future. It is simply the first chapter of adjustment.
What feels unfamiliar now can become routine.
What feels frustrating can become manageable.
What feels exhausting today can turn into steadier energy, clearer thinking, and more stable sleep over time.
You do not have to be perfect at this.
You only have to keep going gently.
Night by night.
Breath by breath.
You are building something that supports your long‑term health.
And that is something to be proud of.
If you found this useful, please feel free to share on social media,
This was written to help people like myself with CPAP and should not be sold.
You can contact me, with feedback here
Email: pdspublishing@live.co.uk
Affiliate Links Included in This Guide
- ResMed F20 Full Face Mask
https://geni.us/4MGFu6s - ResMed AirSense 10 Humidifier Chamber
https://geni.us/Z03Qa - ResMed AirSense 11 Humidifier Chamber
https://geni.us/l7L2aHe - ResMed AirSense 10 Heated Tube (ClimateLineAir)
https://geni.us/pwVwsB - ResMed AirSense 11 Heated Tube (ClimateLineAir 11)
https://geni.us/AEE42 - CPAP Hose Cover
https://geni.us/wYlcD - O2 ring https://geni.us/WHNVxu (Amazon)
- As an Amazon Associate I earn from qualifying purchases.
Starting CPAP: A Complete Real World Beginner’s Guide
From Setup to Sleeping Comfortably — A Simple Step‑by‑Step Guide from A Real CPAP User
Introduction
I’m Really Glad You Found This
If you’re reading this, there’s a very good chance you’re overwhelmed.
I know I certainly was!
Maybe you’ve just been diagnosed with sleep apnea and you’re still trying to process what that even means. Maybe you recently brought a CPAP machine home and it’s sitting on your bedside table right now, quietly waiting for tonight. Maybe you tried it once and already feel discouraged.
You might be thinking:
“I can’t breathe in this thing.”
“This feels unnatural.”
“What if I never get used to it?”
“What if I fail at this?”
Before we go any further, pause.
Take one slow breath in.
And let it out slowly.
Nothing about how you’re feeling right now is unusual.
You are not weak for feeling anxious.
You are not dramatic for feeling unsettled.
You are not failing because it feels hard.
You are human.
I know this because I was exactly where you are.
When I was diagnosed, I felt two things at the same time: relief and fear.
Relief — because there was finally an explanation for the constant exhaustion, the brain fog, the morning headaches, the feeling of never truly feeling rested.
Fear — because I was told I would need a machine to breathe at night.
A machine!
The pickup appointment was efficient. The technician explained the buttons, fitted the mask, adjusted straps, and showed me how to fill the humidifier (which was not included). I nodded along, trying to absorb everything.
Then I went home.
And that night, sitting on the edge of my bed holding the mask in my hands, it all hit me.
This wasn’t theoretical anymore.
This was real.
Honestly it was overwhelming.
The first time I turned the machine on and put the mask to my face, my body reacted instantly. My breathing felt mechanical. The air pressure felt strange. I became hyper‑aware of every inhale and exhale.
Within seconds my thoughts spiralled:
“This isn’t normal.”
“I can’t relax like this.”
“There’s no way I can sleep like this.”
I pulled the mask off.
No one had warned me about that part.
No one had prepared me for the emotional side of starting CPAP — the vulnerability of sleeping with equipment, the anxiety of forced airflow, the strange psychological adjustment of relying on a device to breathe well.
What I eventually learned — slowly, imperfectly — was this:
What I was feeling was completely normal.
The panic was not proof I couldn’t adapt.
The discomfort was not permanent.
The fear was part of the adjustment process.
Gradually, the sharp edges softened.
What felt alarming became tolerable.
What felt tolerable became familiar.
What felt familiar eventually became routine.
This guide is what I wish someone had calmly explained to me during that first week.
No overwhelming medical jargon.
No unrealistic promises.
No pressure to “just get used to it.”
Just steady reassurance and practical steps that move you from fear to confidence — at a human pace.
You don’t have to master this tonight.
You only have to take the next small step.
And then another tomorrow.
Medical Disclaimer
This guide is for informational and educational purposes only.
I am not a physician, sleep specialist, respiratory therapist, or licensed medical professional. The content in this guide is based on personal experience combined with widely available general information about CPAP therapy.
It is not intended to diagnose, treat, cure, or prevent any medical condition.
Always follow the guidance of your healthcare provider regarding pressure settings, equipment adjustments, and treatment decisions. Never change prescribed pressure settings or discontinue therapy without consulting your provider.
If you experience chest pain, severe breathing difficulty, persistent discomfort, or any concerning symptoms, seek medical advice from a qualified healthcare professional.
You are responsible for your own health decisions, and this guide does not replace professional medical care.
PHASE 1 – CALMING THE PANIC
When Everything Feels Overwhelming
The beginning is often the hardest part — not because CPAP is impossible, but because it disrupts something deeply personal: sleep.
Sleep is when we are most vulnerable.
And now you’re being asked to trust a machine during that vulnerable state.
Of course, your nervous system reacts.
Step 1 – You’re Not Weak for Feeling This Way
Let’s say this clearly:
You’ve been told you stop breathing at night.
You’ve been handed medical equipment.
You’ve been expected to adapt quickly.
That is a lot for anyone.
Your brain’s primary job is to keep you safe. When something unfamiliar covers your face and pushes air into your airway, your nervous system evaluates it as a potential threat.
That reaction can look like:
“I can’t relax.”
“This feels wrong.”
“I need to take this off right now.”
That is not failure.
That is your nervous system doing its job.
Your brain is not rejecting CPAP.
It is trying to understand it.
Learning requires repetition.
Right now, your only job is exposure — not perfection.
If you wear it for ten minutes, that is exposure.
If you turn it on and sit upright reading, that is exposure.
If you fall asleep with it for an hour, that is exposure.
I honestly could not put the mask over my face at all so if that’s you then don’t panic.
Each exposure teaches your brain:
“This is safe.”
And safety reduces panic.
Step 2 – Understanding Your Diagnosis Without Spiralling
The language around sleep apnea can sound frightening.
“Moderate.”
“Severe.”
“High AHI.”
“Oxygen desaturation.”
It’s easy for your mind to jump from those words to catastrophic conclusions.
But here’s what those classifications actually mean:
They describe frequency — not doom.
They measure how often breathing is interrupted during sleep.
They do not predict your future.
They do not mean your body is irreparably damaged. They do not mean something terrible is about to happen.
Sleep apnea is common.
Millions of people have it.
It is highly treatable.
CPAP therapy is one of the most researched and effective treatments in sleep medicine.
You were not diagnosed because something is hopeless.
You were diagnosed because something is manageable — and now it’s being managed.
Instead of thinking:
“This is severe. This is terrible.”
Try shifting to:
“This is treatable. And I am treating it.”
That shift alone lowers anxiety.
You are not ignoring the problem.
You are addressing it.
That matters.
It might not feel like it just now, but I promise you that you are now in a much better position.
Step 3 – Why the Pickup Appointment Feels So Fast
Almost everyone has the same experience.
You go to collect your CPAP machine. The technician explains the buttons, shows you how to assemble the mask, talks about humidity settings, maybe mentions compliance requirements — and then it’s over.
You walk out with a machine in a bag.
Later that evening, you realise something uncomfortable:
You don’t remember half of what was said.
This is incredibly common. My experience was, where do these straps go? How do I get the mask on, where does this tube attach. It felt desperately hopeless.
When we’re stressed, our brains prioritise emotional processing over memory storage. Being told you stop breathing at night — even calmly — activates stress. Stress reduces information retention.
It doesn’t mean you weren’t paying attention.
It doesn’t mean you’re bad with instructions.
It means you were processing something significant.
You are not behind.
You are learning something new, and learning happens through repetition — not one appointment.
If you need to watch tutorials, reread instructions, or ask questions later, that’s not incompetence. That’s reinforcement. That’s normal.
Step 4 – Lowering the Bar for Success
Many new CPAP users silently create an impossible rule:
“If I can’t wear it all night immediately, I’m failing.”
Beware of this and take a moment to address this, this is super important and completely not true.
That belief creates pressure.
Pressure creates anxiety.
Anxiety makes sleep harder.
So let’s remove that rule entirely.
Tonight, success might be:
20 minutes.
45 minutes.
One sleep cycle.
Putting it back on after waking up.
For me it was simply putting the mask on my face for a few seconds.
All of that counts.
Adaptation is not about intensity. It’s about consistency.
Wearing it for a short period every night teaches your nervous system that the mask is not a threat. Forcing eight straight hours on night one often backfires.
Small, repeatable wins build long‑term success.
Lowering the bar doesn’t lower your standards.
It builds resilience.
But this is where I can really help.
What I did for a few days was just attempt to wear the mask for 30 seconds at a time while sitting up in any other room than your bedroom and watching TV as a distraction.
This alone massively took the pressure off me mentally and actually wearing it just for a few minutes sat up during the day was the key to everything.
Step 5 – Managing Claustrophobia Gently
Claustrophobia is one of the most common early reactions to CPAP.
It is not weakness.
It is not immaturity.
It is your brain reacting to perceived loss of control.
When something covers your nose or face and alters airflow, your nervous system can interpret it as confinement.
The solution is gradual exposure — not force.
Once you have grown comfortable with wearing during the day,
Instead of trying to fall asleep immediately:
Sit upright.
Keep the lights on.
Put the mask on for one minute.
Breathe slowly and deliberately.
Then take it off.
Do this daily.
Then extend it to two minutes.
Then five.
You are not trying to prove anything. You are retraining your nervous system.
Each calm repetition sends a signal:
“This is safe. I can remove it anytime.”
Control reduces panic.
And repetition builds calm.
If I could only give one piece of advice, then this would be it.
PHASE 2 – MAKING IT MORE COMFORTABLE
Reducing the Friction
If you’re reading this section, it means you didn’t quit.
That matters. Even if you still feel like you are failing, you simply are not,
Most successful long‑term CPAP users did not succeed immediately. They struggled. They adjusted. They experimented. They learned.
They stayed.
This phase is about reducing the small annoyances that create resistance.
Step 6 – Taking the Mask Off in Your Sleep
You may wake up in the middle of the night and realise your mask is on the pillow beside you.
Your first thought might be:
“I failed.”
You didn’t.
Your unconscious brain removes unfamiliar objects during sleep. Especially in the early weeks.
Think of it this way:
Your waking brain agreed to wear the mask.
Your sleeping brain hasn’t fully caught up yet.
Each night you wear it — even partially — your brain gathers evidence:
“That was safe.”
“I could breathe.”
“Nothing bad happened.”
Over time, familiarity reduces removal.
If you wake up and it’s off, calmly put it back on if you can.
No frustration.
No self‑criticism.
Just repetition.
It’s no big deal, eventually one morning you will wake up with the mask on. Reward yourself on that day!
Step 7 – Stop Overtightening the Mask
When you feel or hear a leak, your instinct may be to tighten the straps.
Tighter feels more secure.
But tighter is not always better.
Most CPAP masks are designed to inflate slightly with air pressure. That inflation helps create the seal. If you overtighten, you can actually distort the cushion and increase leaks.
Overtightening also creates:
Pressure marks
Facial soreness
Headaches
More resistance to wearing it
Instead of pulling straps tighter, try:
Reseating the mask gently
Adjusting while lying down
Allowing the cushion to inflate naturally
Comfort improves compliance.
Force increases frustration.
What I do is put the mask in position on my face and then turn on the air, I feel this gives me a better seal.
Step 8 – Mask Leaks Are Mechanical, Not Personal
Leaks are one of the most common frustrations.
They can sound loud.
They can blow air into your eyes.
They can wake your partner.
It’s easy to interpret leaks emotionally:
“I can’t even wear this properly.”
But leaks are mechanical problems.
And mechanical problems have mechanical solutions.
It may mean:
The mask size isn’t ideal.
The cushion needs replacing.
The straps need minor adjustment.
Your sleeping position shifted.
None of those mean you’re incapable.
You’re learning equipment.
Learning always involves adjustment.
I currently use a ResMed F20 as its super simple.
This is purely personal preference but don’t put up with leaks.
There are tons of options to try. I just want something that covers my nose and mouth with a good seal.
Check out the ResMed F20 mask here on Amazon
(Click the blue links and it takes you to Amazon)
https://geni.us/4MGFu6s (Amazon)
(As an Amazon associate, I earn from qualifying purchases)
And if strap marks are a problem check out this solution,
Pad A Cheek
https://www.padacheek.com
Step 9 – Dry Mouth and Humidity Issues
Waking up with a dry mouth can feel discouraging.
Common causes include:
Mouth breathing
Low humidity settings
Dry bedroom air
Instead of changing everything at once, adjust one variable at a time.
Increase humidity slightly.
Observe for a few nights.
Then reassess.
Systematic adjustment builds confidence.
You move from feeling helpless to feeling capable.
And that psychological shift is powerful.
This hurdle takes consistency to overcome.
When I receive my CPAP machine (Resmed Airsense 10) It did not include the humidifier chamber, once I added this it greatly reduced dryness by adding a small amount of humidity to the air,
Check out the ResMed AirSense 10 and 11 Humidifiers below.
https://geni.us/Z03Qa (Amazon) AirSense10
https://geni.us/l7L2aHe (Amazon) AirSense 11
As an Amazon Associate, I earn from qualifying purchases)
The final piece of the puzzle for me though was purchasing a heated tube.
A heated CPAP tube helps prevent condensation (“rainout”) in the hose while maintaining consistent warm airflow, which reduces dryness, nasal irritation, and sudden bursts of water in the mask for a more comfortable night’s sleep.
You can control the air temperature, and this really helps with comfort.
Check out the heated tube below
https://geni.us/pwVwsB (Amazon) ResMed AirSense 10
https://geni.us/AEE42 (Amazon) ResMed AirSense 11
(As an Amazon Associate, I earn from qualifying purchases)
Step 10 – Air in the Stomach (Aerophagia)
Some people experience bloating or mild stomach discomfort in the early weeks.
This can happen when air is swallowed during adaptation.
It often improves as:
Your body adjusts to pressure
Your breathing becomes more relaxed
Your anxiety decreases
Mild early discomfort does not mean damage.
It usually means adaptation.
If it persists or is severe, consult your provider — but early temporary bloating is common and often resolves naturally.
Let’s just say a little extra gas is inevitable!
Step 11 – Hose Management Matters More Than You Think
The hose can feel surprisingly intrusive.
Dragging across the bed.
Pulling when you turn.
Getting tangled.
Small setup changes can make a big difference.
You Could Try:
Routing the hose above your head
Using a hose holder
Clipping it to the headboard
Positioning it so it moves freely
When physical resistance decreases, emotional resistance often decreases too.
Comfort is cumulative.
What I do to avoid “Rainout” is put the machine near the floor lower than my sleeping position, along with a heated tube this helps with “Rainout”
Rainout is when warm, humidified air from your CPAP cools inside the hose and turns back into water droplets, causing moisture to collect in the tubing or mask. You don’t want rainout because it can lead to gurgling noises, water splashing into your mask, disrupted sleep, and reduced comfort throughout the night.
If you don’t have a heated tube a cheaper option is a hose cover to keep the tube a little warmer. This may be enough depending on your settings and set up to avoid rainout,
Check out the cover I use below
https://geni.us/wYlcD (Amazon)
(As an Amazon associate, I earn from qualifying purchases)
PHASE 3 – BUILDING CONFIDENCE
When It Starts Feeling Manageable
At some point — often quietly — something begins to shift.
The panic isn’t as sharp.
The mask doesn’t feel quite as foreign.
You stop bracing yourself every time you turn the machine on.
This phase is subtle but important.
You move from reacting…
to participating.
Instead of thinking, “I hope I survive this night,”
you begin thinking, “How can I make this work better?”
That shift is confidence forming.
Step 12 – Create a Simple Night Routine
Predictability calms the nervous system.
When your brain knows what comes next, it relaxes more easily.
Instead of treating CPAP as an interruption, integrate it into a consistent pre‑sleep sequence.
For example:
- Wash your face
- Fill the humidifier
- Check the mask cushion
- Put the mask on
- Turn the machine on
- Take one slow breath in, one slow breath out
Follow the same order each night.
Over time, the routine itself becomes a cue for sleep.
The mask stops feeling like a disruption.
It becomes part of the ritual.
And rituals are calming.
Step 13 – Keep Cleaning Simple and Sustainable
In the beginning, it’s easy to become overly strict.
You might feel like you need to deep clean everything constantly or you’re “doing it wrong.”
Perfection is not required.
Sustainability is.
A simple approach works well:
• Quick wipe of the mask cushion daily
• Regular wash of mask and tubing
• Replace worn cushions and filters as needed
You don’t need elaborate systems.
You need repeatable systems.
When maintenance feels manageable, resistance decreases.
Here’s what I do.
I clean the hose every 3 days, run some dish soap and water through and a cpap cleaning hose brush.
For the humidity chamber I do this daily. I clean with water and dish soap and use a toothbrush to clean the inner.
For the mask cushion I use a bar of soap (Imperial leather brand)
What I found at first is that if I used a CPAP wipe or forgot to clean the mask all together it led to more leaks. This is due to the mask sliding.
Washing with a bar of soap (daily) gives the cushion surface the correct grip again)
Step 14 – Understand Just Enough
You don’t need to become a sleep technician.
But understanding a few key concepts reduces helplessness.
For example:
AHI – how many breathing interruptions occur per hour
Leak rate – whether your mask is sealing effectively
Humidity – how moisture affects comfort
When you understand what these mean, you stop guessing.
You start interpreting.
You move from:
“Something feels wrong.”
To:
“I know what this number means.”
Knowledge replaces uncertainty.
And uncertainty is what fuels anxiety.
Step 15 – Tracking Progress Without Obsessing
Most CPAP machines track basic data:
• AHI
• Leak rate
• Usage hours
You may view this on the machine itself or through software platforms like SleepHQ or OSCAR.
Seeing improvement can be incredibly encouraging.
Lower AHI numbers.
Longer usage hours.
Fewer leaks.
Data becomes reassurance.
But here’s the balance:
Look at trends — not single nights.
Sleep varies.
Stress affects results.
Illness affects results.
Travel affects results.
One imperfect night does not erase progress.
Consistency over weeks matters more than perfection over one evening.
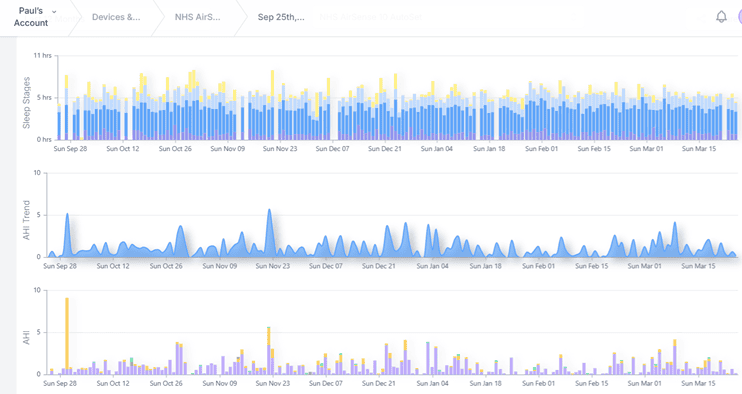
Sleep HQ has a user-friendly dashboard that shows your daily information and trend data over time.
There is a free trial, and the community is incredibly helpful.
You can visit SleepHQ here, https://www.sleephq.com/
Daily Dashboard (My data)
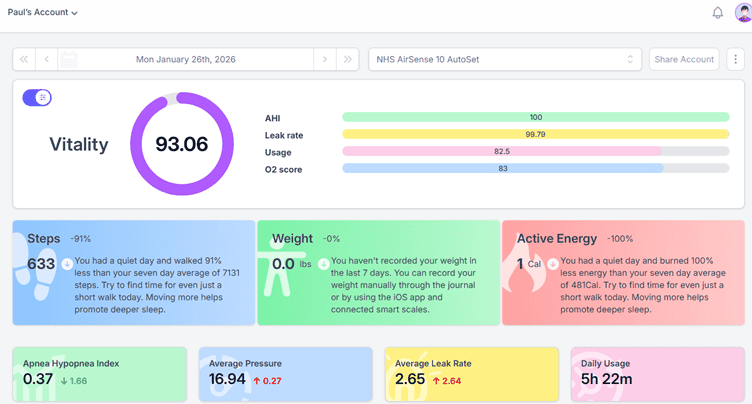
Trend data.
Step 16 – Notice Subtle Improvements
Improvements are sometimes quiet.
You may not wake up feeling dramatically different.
Instead, you might notice:
You’re thinking more clearly mid‑morning.
You’re not reaching for caffeine as desperately.
Your mood feels steadier.
You’re not crashing in the afternoon.
These changes can be gradual.
Pause when you notice them.
Your brain needs to register success.
When you consciously acknowledge improvement, motivation strengthens.
Step 17 – Let Yourself Feel Hopeful
There may come a morning — unexpectedly — when you wake up and think:
“I actually feel… okay.”
Not euphoric.
Not transformed.
Just… okay.
Rested enough. Clear enough.
That moment is powerful.
Because it proves something:
This is working.
CPAP shifts from being a burden you tolerate…
to support your value.
And that psychological transition changes everything.
PHASE 4 – LONG‑TERM CONFIDENCE
When It Becomes Normal
There will be a night when you put the mask on without debating it.
No internal argument.
No tension in your shoulders.
No countdown in your head.
You just put it on.
Like brushing your teeth.
That’s not surrender.
That’s adaptation.
Step 18 – From Patient to Capable
At this stage, something subtle changes in identity.
You no longer feel like someone “dealing with a condition.”
You feel like someone managing their health.
You understand your machine.
You know how to adjust comfort settings.
You recognise normal variations.
You feel capable.
Capability replaces fear.
Step 19 – Bad Nights Still Happen
Even experienced users have rough nights.
Stress.
Illness.
Congestion.
Travel.
Life.
A single bad night does not undo months of consistency.
Progress is not erased by imperfection.
Stay steady.
Consistency over time is what matters. Don’t blame CPAP for every future symptom you get. They might have happened anyway,
Step 20 – Travel With Confidence
The first time you travel with your CPAP, it may feel awkward.
You may feel self‑conscious carrying it.
But something interesting happens over time:
You realise how much better you sleep with it.
You start packing it automatically.
You prioritise your rest.
That’s growth.
You move from embarrassment to ownership.
Also, I will add that CPAP machines do not count as carry on luggage, so take onboard with you alongside your carry on luggage,
Step 21 – Letting Go of Shame
There is nothing shameful about treating a medical condition.
Millions of people use CPAP.
Athletes. Professionals. Parents. Partners.
Health maintenance is not weakness.
It is responsibility.
Confidence replaces self‑consciousness when you remember:
You are taking care of yourself.
Step 22 – Look How Far You’ve Come
Think back to the first night.
The uncertainty.
The panic.
The doubt.
Now look at where you are.
You stayed.
You adjusted.
You learned.
That is resilience.
Not dramatic resilience.
Quiet resilience.
And quiet resilience is powerful.
Step 23 – Energy Returning
As breathing stabilises during sleep:
Oxygen levels stabilise.
Micro‑awakenings decrease.
Deep sleep becomes more consistent.
The benefits compound gradually.
You may feel:
Clearer thinking
More stable mood
Improved concentration
Greater patience
Energy doesn’t always return in a dramatic rush.
Sometimes it builds quietly.
But it builds.
Step 24 – When You Know It’s Working
There is often a simple moment.
A quiet morning.
You wake up and think:
“I’m glad I stuck with this.”
That thought signals a turning point.
The machine is no longer the enemy.
It is support.
Step 25 – This Is Sustainable
CPAP is not a temporary test of endurance.
It becomes routine.
Normal.
Integrated.
Like wearing glasses.
Like using a seatbelt.
Like brushing your teeth.
At first it feels intrusive.
Eventually, it just feels sensible.
And normal is powerful.
Step 26 – You’re Stronger Than You Thought
You faced something that scared you.
You adapted to something uncomfortable.
You didn’t quit on the hard nights.
That’s strength.
Not loud strength.
Steady strength.
And steady strength lasts.
Step 27 – Hope Moving Forward
The intensity of the beginning does not last forever.
Panic softens.
Equipment becomes familiar.
Resistance fades.
Confidence replaces doubt.
Adaptation is one of the most reliable traits of the human nervous system.
Given repetition and safety, it adjusts.
You are adjusting.
Even when it feels slow.
Even when it feels imperfect.
Adaptation works.
Step 28
What If CPAP Isn’t Working and I Still Feel Tired?
If you’re using your CPAP consistently but still waking up tired, foggy, or discouraged, there is one simple step that can give you real clarity:
Start tracking your overnight oxygen levels.
The entire purpose of CPAP therapy is to keep your airway open so your oxygen stays stable throughout the night. When oxygen repeatedly drops — even briefly — your body goes into stress mode. Your heart rate increases. Your brain partially wakes. Deep sleep gets disrupted. And the result is simple: you still feel exhausted.
You cannot feel oxygen levels.
You cannot guess oxygen stability.
You have to measure it.
That’s where an O₂ ring becomes incredibly valuable.
Unlike most smartwatches, which measure oxygen only periodically, a dedicated O₂ ring tracks your oxygen continuously throughout the entire night. It stays securely on your finger and records detailed trends, including short desaturations that can easily be missed otherwise.
Instead of lying in bed wondering:
“Is this working?”
“Why am I still tired?”
“Is something wrong?”
You wake up with answers.
You can see:
- Whether your oxygen stayed stable
- Whether drops are still happening
- Whether things are improving over time
That clarity alone reduces anxiety.
For me personally, this was the turning point. I stopped guessing and started measuring. When I began monitoring my oxygen nightly, I could actually see progress. As my oxygen levels became more stable, I started feeling clearer and more consistent during the day.
It wasn’t dramatic.
It wasn’t instant.
But it was measurable.
And measurable progress builds confidence.
If you are serious about understanding whether your CPAP therapy is truly working, an O₂ ring is one of the most empowering tools you can add. It turns uncertainty into data. It turns doubt into direction.
This vibrates if your blood oxygen drops below a certain level, You can turn this off as well though.
What I did at the beginning of my CPAP journey is I wore the 02 Sensor overnight with out cpap.
Here is the result (First Night No CPAP)
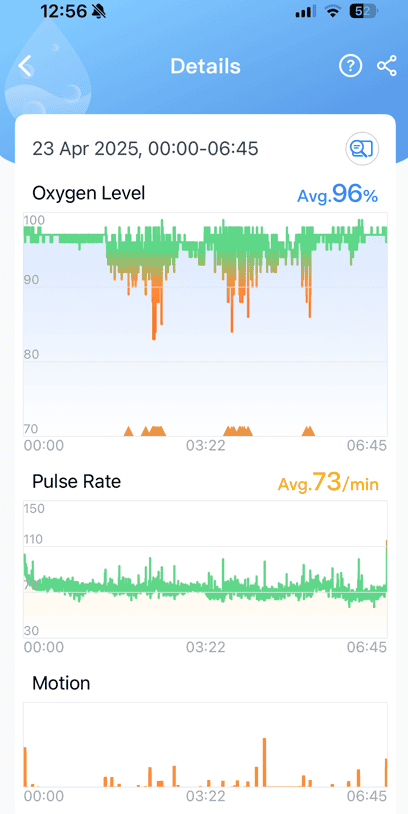
And here is my result today, (11 months apart)
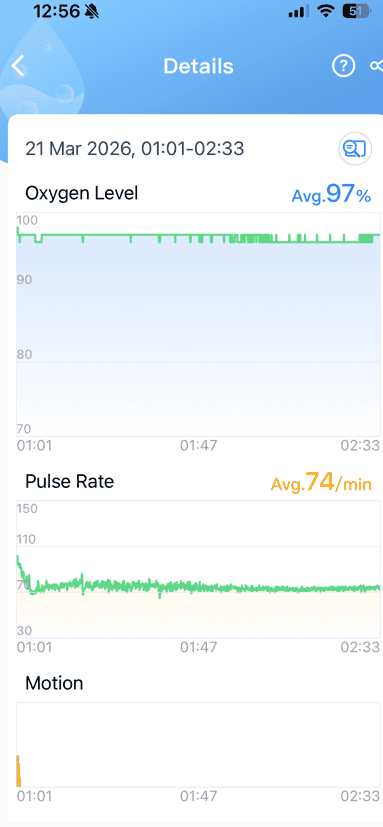
Check out the O2 ring here https://geni.us/WHNVxu (Amazon)
Sometimes the difference between “CPAP isn’t working” and “CPAP is helping” is simply having the right information in front of you.
An O₂ ring gives you that information.
The combination of this and the helpful forum on SLEEPHQ and all the data got me to this point.
Helpful Resources
SleepHQ
https://sleephq.com
OSCAR (Free CPAP Data Software)
https://www.sleepfiles.com/OSCAR/
Pad A Cheek
https://www.padacheek.com
CPAP Reviews (Nick)
https://www.youtube.com/@CPAPReviews
TheLankyLefty27
https://www.youtube.com/@TheLankyLefty27
FreeCPAPAdvice
https://www.youtube.com/@FreeCPAPAdvice
Final Words
If you take nothing else from this guide, take this:
The discomfort of the beginning is not a prediction of the future. It is simply the first chapter of adjustment.
What feels unfamiliar now can become routine.
What feels frustrating can become manageable.
What feels exhausting today can turn into steadier energy, clearer thinking, and more stable sleep over time.
You do not have to be perfect at this.
You only have to keep going gently.
Night by night.
Breath by breath.
You are building something that supports your long‑term health.
And that is something to be proud of.
If you found this useful, please feel free to share on social media,
This was written to help people like myself with CPAP and should not be sold.
You can contact me, with feedback here
Email: pdspublishing@live.co.uk
Affiliate Links Included in This Guide
- ResMed F20 Full Face Mask
https://geni.us/4MGFu6s - ResMed AirSense 10 Humidifier Chamber
https://geni.us/Z03Qa - ResMed AirSense 11 Humidifier Chamber
https://geni.us/l7L2aHe - ResMed AirSense 10 Heated Tube (ClimateLineAir)
https://geni.us/pwVwsB - ResMed AirSense 11 Heated Tube (ClimateLineAir 11)
https://geni.us/AEE42 - CPAP Hose Cover
https://geni.us/wYlcD - O2 ring https://geni.us/WHNVxu (Amazon)
- As an Amazon Associate I earn from qualifying purchases.





